PARASITIC DERMATOSES : DEMODICOSIS - CANINE
- At a glance
- WHAT DOES IT LOOK LIKE?
- WHAT ELSE LOOKS LIKE THIS?
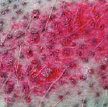
- HOW DO I DIAGNOSE IT?
- HOW DO I MANAGE IT?
- COMMENTS
AT A GLANCE
- An overgrowth of the skin commensal mite Demodex canis
- 2 other mites, Demodex injai (long-bodied) and Demodex cornei (short-bodied) may also cause disease.
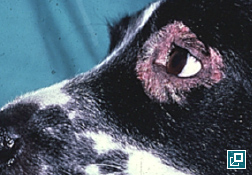
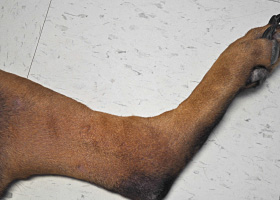
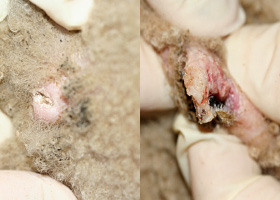
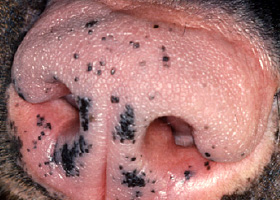
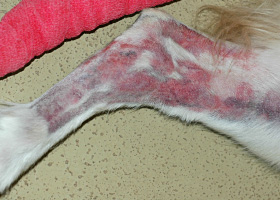
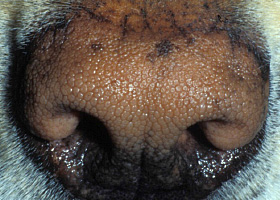
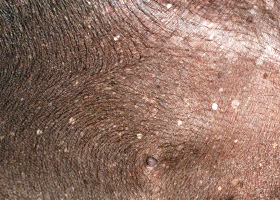
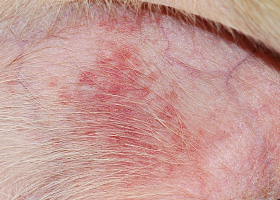
WHAT DOES IT LOOK LIKE?
- 3 clinical forms:
- Localized has no more than 5 lesions, up to 2.5 cm
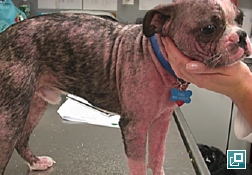
- Juvenile onset generalized demodicosis has multiple (> 5) lesions, involves entire body regions, or more than 1 foot, and begins at less than 2 years of age
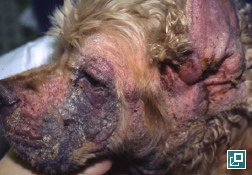
- Adult-onset generalized demodicosis occurs in dogs > 2 years; typically aged dogs
- Lesions range from regional to generalized alopecia, scaling, erythema, hyperpigmentation and/or comedones
- Concurrent folliculitis, furunculosis or cellulitis
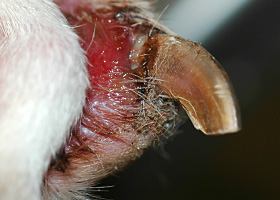
- Demodicosis is a common cause of pododermatitis
WHAT ELSE LOOKS LIKE THIS?
- Bacterial folliculitis, furunculosis, cellulitis
- Dermatophytosis
- Pemphigus foliaceus
HOW DO I DIAGNOSE IT?
- Deep skin scraping; multiple sites if generalized
- Acetate Tape Impression of squeezed skin; particularly for face and feet
- Trichogram−mites can be pulled out of follicles along with the hairs
- Biopsy occasionally needed−especially for chronic lesions on the feet and in Shar-Pei dogs
- Cytology +/- culture and susceptibility to evaluate secondary bacterial infection
How do I treat it?
- Observation and recheck in 30 days
- Consider topical benzoyl peroxide or rotenone
- If lesions progress, treat as for generalized
- Acaricidal therapy and treatment of secondary bacterial infection
- In dogs with adult-onset generalized demodicosis evaluate for underlying diseases or immunomodulatory therapies
- Topical amitraz
- Systemic high dose, high frequency macrocyclic lactone/ avermectins.
Note that these macrocyclic lactone/ avermectins protocols are not approved but based on common usage and the veterinary medical literature - Prior to treatment with macrocyclic lactone/ avermectins, dogs should be tested heartworm negative and evaluated for possible neurotoxicity by test dosing or determination of ABCB1- delta1 (MDR-1) gene status.
AVERMECTIN NEUROTOXICITY: mydriasis, ataxia, lethargy, tremors, blindness and death in sensitive dogs.
Note toxicity has occurred in dogs with normal ABCB1- delta1 gene function
Do not use spinosad concurrently with high dose, high frequency macrocyclic lactone/ avermectin therapy. P-glycoprotein inhibitors, such as ketoconazole or ciclosporin, if given concurrently, increase the likelihood of adverse effects
| MEDICATION | DOSE | WARNINGS |
|---|---|---|
| Amitraz |
|
|
| Ivermectin |
|
|
| Milbemycin |
|
|
| Moxidectin |
|
|
| Doramectin |
|
|
Re-scrape every 14 to 28 days and maintain acaricidal treatment for 28 days beyond second negative skin scrape. Monitor progress by recording density and ratio of adult mites, nymphs, larvae and eggs, live or dead.
Antibiotic therapy, ideally based on culture and susceptibility, until clinical and cytologic resolution of secondary bacterial infection.
COMMENTS
- Most common cause of treatment failure is lack of duration of treatment.
- If numbers of eggs, larvae and live mites do not progressively decrease consider changing the frequency of topical or spot-on treatments, increasing the dose of oral avermections, or changing to an alternative therapy.
- Adult onset generalized may require life-long therapy. Dogs are considered cured it they remain mite free 1 year past the last treatment.
- Spay females as soon as possible as the disease may flare with estrous.
- Recommend that all dogs with juvenile onset generalized demodicosis be neutered as this form appears to have a genetic predisposition.
References
- 1 1. Miller WH, Griffin CE. Campbell K. eds. Muller and Kirk’s Small Animal Dermatology 7th ed. Saunders, 2013: 125. 311-313
- 2. Nuttall T. Harvey G. McKeever. PJ. Skin Diseases of the Dog and Cat. 2009. 275-276
abscess
A discrete swelling containing purulent material, typically in the subcutis
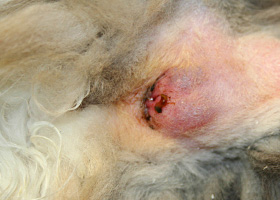
Perianal abscess in a dog
alopecia
Absence of hair from areas where it is normally present; may be due to folliculitis, abnormal follicle cycling, or self-trauma
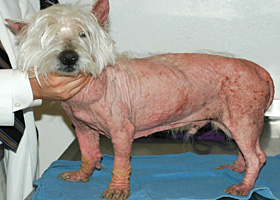
Extensive alopecia secondary to cutaneous epitheliotropic lymphoma
alopecia (“moth-eaten”)
well-circumscribed, circular, patchy to coalescing alopecia, often associated with folliculitis
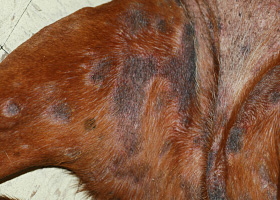
“Moth-eaten” alopecia secondary to superficial bacterial folliculitis
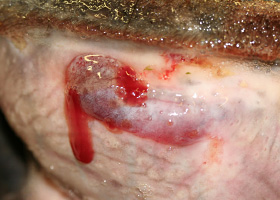
hemorrhagic bullae
Blood-filled elevation of epidermis, >1cm
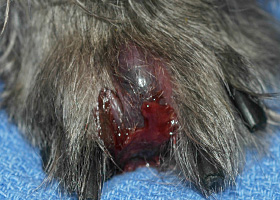
Interdigital hemorrhagic bulla in a dog with deep pyoderma and furunculosis
comedo
dilated hair follicle filled with keratin, sebum
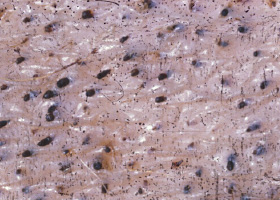
Comedones on the ventral abdomen of a dog with hypercortisolism
crust
Dried exudate and keratinous debris on skin surface
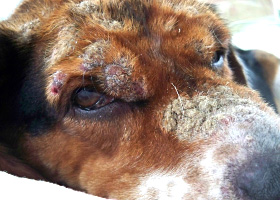
Multifocal crusts due to pemphigus foliaceus
epidermal collarettes
Circular scale or crust with erythema, associated with folliculitis or ruptured pustules or vesicles
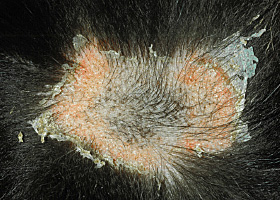
Epidermal collarettes in a dog with Staphylococcus superficial bacterial folliculitis
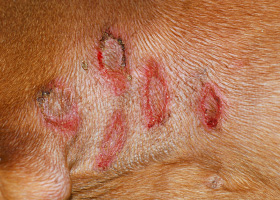
erosion
Defect in epidermis that does not penetrate basement membrane. Histopathology may be needed to differentiate from ulcer.
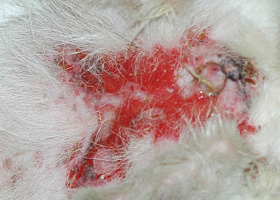
Erosions in a dog with vasculitis
erythema
Red appearance of skin due to inflammation, capillary congestion
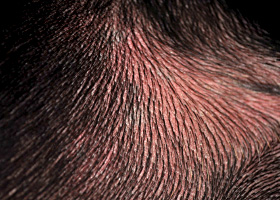
Erythema in a dog with cutaneous drug eruption
eschar
Thick crust often related to necrosis, trauma, or thermal/chemical burn
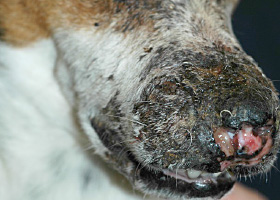
Eschar from physical trauma
excoriation
Erosions and/or ulcerations due to self-trauma
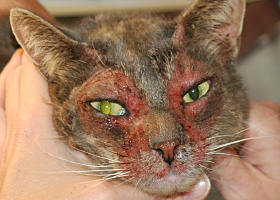
Excoriations in a cat with atopic dermatitis
fissure
Excessive stratum corneum, confirmed via histopathology. This term is often used to describe the nasal planum and footpads.
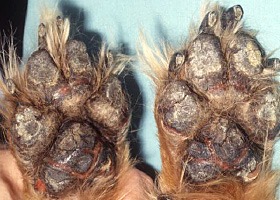
Fissures of the footpads in a dog with superficial necrolytic dermatitis
fistula
Ulcer on skin surface that originates from and is contiguous with tracts extending into deeper, typically subcutaneous tissues
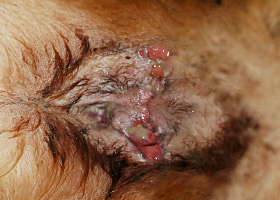
Perianal fistulas in a dog
follicular casts
Accumulation of scale adherent to hair shaft
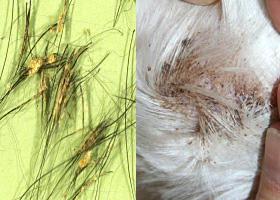
Follicular casts surrounding hairs from a dog with hypothyroidism
hyperkeratosis
Excessive stratum corneum, confirmed via histopathology. This term is often used to describe the nasal planum and footpads.
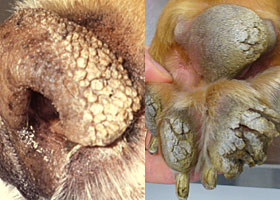
Idiopathic hyperkeratosis of the nasal planum (left) and footpads (right)
hyperpigmentation
Increased melanin in skin, often secondary to inflammation
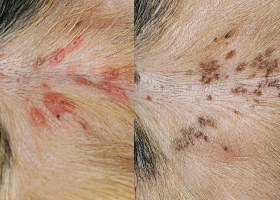
Inflammatory lesions (left) resulting in post-inflammatory hyperpigmentation (right)
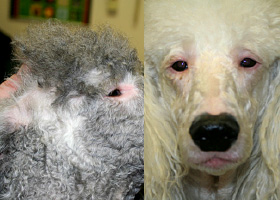
hypotrichosis
Lack of hair due to genetic factors or defects in embryogenesis.

Congenital hypotrichosis in chocolate Labrador puppies.
lichenification
Thickening of the epidermis, often due to chronic inflammation resulting in exaggerated texture
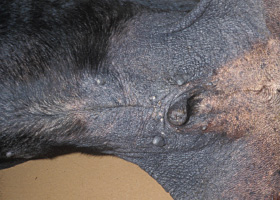
Lichenification of skin in a dog with chronic atopic dermatitis and Malassezia dermatitis
macule
Flat lesion associated with color change <1cm
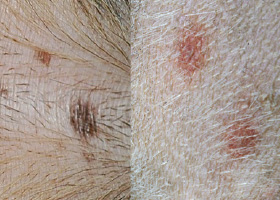
Pigmented macule (left) Erythematous macule (right)
melanosis
Increased melanin in skin, may be secondary to inflammation.
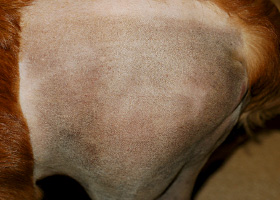
Post inflammatory hyperpigmentation of this dog’s thigh
miliary
Multifocal, papular, crusting dermatitis; a descriptive term, not a diagnosis
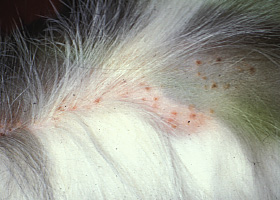
Miliary dermatitis in a flea allergic cat
morbiliform
A erythematous, macular, papular rash; the erythematous macules are typically 2-10 mm in diameter with coalescence to form larger lesions in some areas
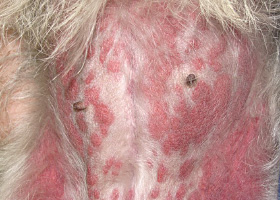
Morbiliform eruptions in a dog with a cutaneous drug reaction
onychodystrophy
Abnormal nail morphology due to nail bed infection, inflammation, or trauma; may include: Onychogryphosis, Onychomadesis, Onychorrhexis, Onychoschizia
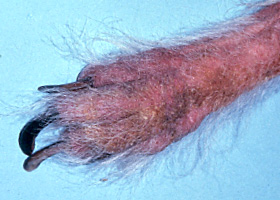
Onychodystrophy in dog with chronic allergies
onychogryphosis
Abnormal claw curvature; secondary to nail bed inflammation or trauma

Onychogryphosis in a dog with symmetric lupoid onychodystrophy
onychomadesis
Claw sloughing due to nail bed inflammation or trauma
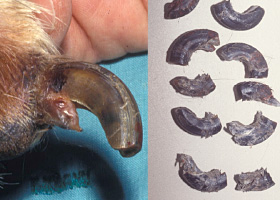
Onychomadesis in a dog with symmetric lupoid onychodystrophy
onychorrhexis
Claw fragmentation due to nail bed inflammation or trauma
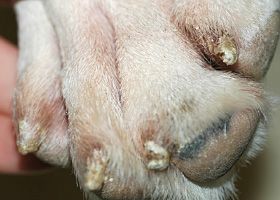
Onychorrhexis in a dog with symmetric lupoid onychodystrophy
onychoschizia
Claw splitting due to nail bed inflammation or trauma
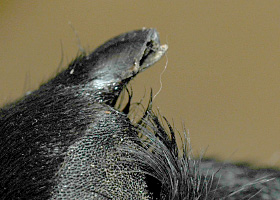
Onychoschizia in a dog with symmetric lupoid onychodystrophy
patch
Flat lesion associated with color change >1cm
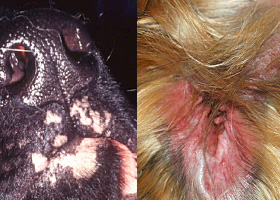
Hypopigmented patch (left), erythematous patch (right)
petechiae
Small erythematous or violaceous lesions due to dermal bleeding
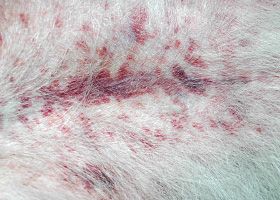
Petechiae in a dog with cutaneous vasculitis
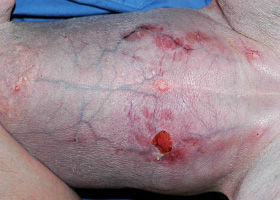
phlebectasia
Venous dilation; most commonly associated with hypercortisolism
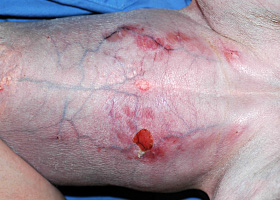
Phlebectasia and cutaneous atrophy due to hypercortisolism in a dog
plaques
Flat-topped elevation >1cm formed of coalescing papules or dermal infiltration
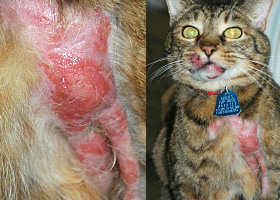
Plaques in a cat with cutaneous lymphoma
pustule
Raised epidermal infiltration of pus
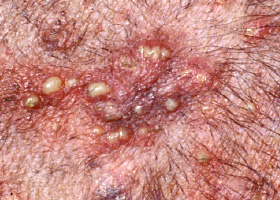
Pustules on the abdomen of a dog with superficial staphylococcal pyoderma.
scale
Accumulation of loose fragments of stratum corneum
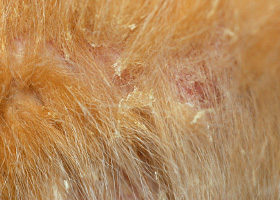
Loose, large scales due to ichthyosis in a Golden Retriever
scar
Fibrous tissue replacing damaged cutaneous and/or subcutaneous tissues
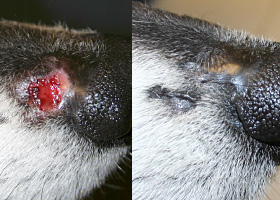
Scarring (right) following the healing of an ulcer (left) in a dog with sterile nodular dermatitis
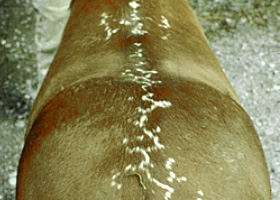
serpiginous
Undulating, serpentine (snake-like) arrangement of lesions

Serpiginous urticarial lesions on a horse
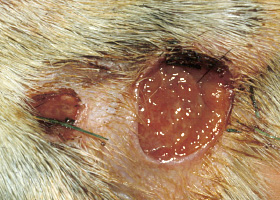
telangiectasia
Permanent enlargement of vessels resulting in a red or violet lesion (rare)
Telangiectasia in a dog with angiomatosis
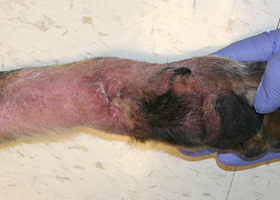
ulcer
A defect in epidermis that penetrates the basement membrane. Histopathology may be needed to differentiate from an erosion.
Ulcerations of the skin of a dog with vasculitis.
urticaria
Wheals (steep-walled, circumscribed elevation in the skin due to edema ) due to hypersensitivity reaction

Urticaria in a horse
vesicle
Fluid-filled elevation of epidermis, <1cm
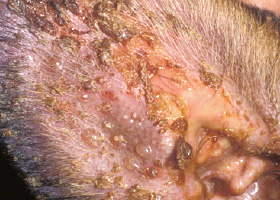
Vesicles and bullae on ear pinna due to bullous pemphigoid
wheal
Steep-walled, circumscribed elevation in the skin due to edema

Wheals associated with intradermal allergy testing in a horse