CONGENITAL & HEREDITARY DERMATOSES : SEBACEOUS ADENITIS
- At a glance
- WHAT DOES IT LOOK LIKE?
- WHAT ELSE LOOKS LIKE THIS?
- HOW DO I DIAGNOSE IT?
- HOW DO I MANAGE IT?
- COMMENTS
AT A GLANCE
- An inflammatory disease that causes the destruction of sebaceous glands
- Leads to scaling and progressive loss of hair
- Uncommon in dogs; also very rare reports in cats and rabbits
- Highest incidence is in young to middle aged animals
- Breed predilections include the Standard Poodle, Hungarian vizsla, Akita, German shepherd dog, Samoyed, Belgian sheepdog and Havanese
- Primarily a cosmetic disease
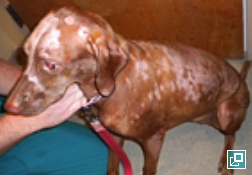
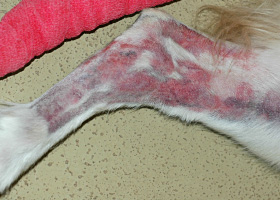
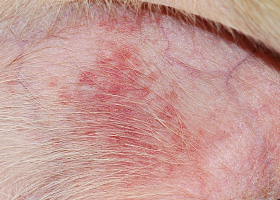
What Does It Look Like?
- Often affects dorsal back and neck in addition to head, face, ears and tail
- Lesions vary from localized to generalized over the body
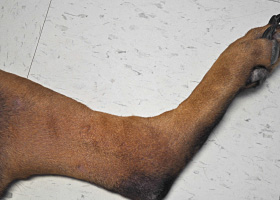
- Short-coated dogs:
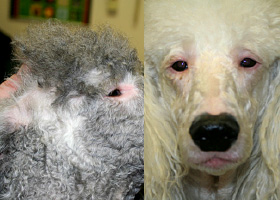
- Long-coated dogs:
- Hair may become lighter or darker or may change from curly to wavy or straight (poodles)
- Dull, brittle haircoat
- Diffuse alopecia is common
- Undercoat is often lost while primary hairs are sparred
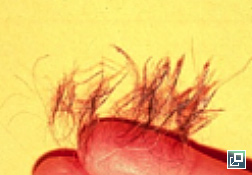
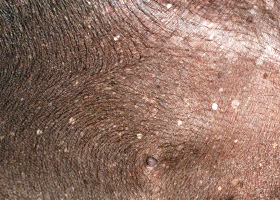
- Scales often adhere to the hairs forming follicular casts
- Other clinical signs may include
- Hyperpigmentation
- Lichenification
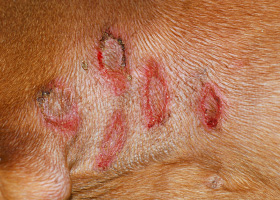
- Secondary superficial or deep pyoderma and associated pruritus
- Otitis externa
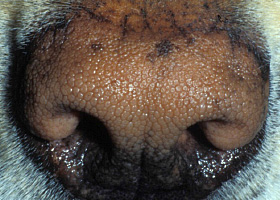
- Greasy skin and haircoat +/- malodor
What Else Does it Look Like?
- Superficial pyoderma
- Demodicosis
- Dermatophytosis
- Follicular dysplasias
- Endocrinopathies- hypothyroidism, hypercortisolism
- Primary seborrhea
- Vitamin A-responsive dermatosis
- Ichthyosis
HOW DO I DIAGNOSE IT?
- History and clinical signs
- Skin scrapings to rule out demodicosis
- Fungal culture to rule out dermatophytosis
- Skin cytology/bacterial culture and susceptibility if indicated
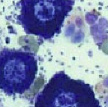
- Biopsy for dermatohistopathology
- Early Lesions
- Discrete granulomas in areas of sebaceous glands
- No involvement of other adnexa
- Chronic Lesions
- Fibrosis replaces absent sebaceous glands
- Hyperkeratosis and follicular plugging may be seen
- Early Lesions
How Do I Manage It?
- Mild cases
- Oral omega-3 and/or omega-6 supplementation daily
- Topical therapy- keratolytic shampoos and emollient rinses/humectants every 2-4 days
- Severe cases
- High doses of oral fatty acid supplementation daily
- Propylene glycol in water (50-70%) spray or water based moisturizing spray daily
- Baby or mineral oil soaks (2-3 hours) followed by bathing to remove excess oil repeated weekly until condition has improved, then every 2-4 weeks for maintenance
- Additional medications
- Vitamin A
- 1000 IU/kg by mouth every 24 hours
- Tetracycline / Niacinamide
- Dogs weighing less than 10kg- 250mg of each by mouth every 8 hours
- Dogs weighing more than 10kg- 500mg of each by mouth every 8 hours
- Prednisone
- 2 mg/kg by mouth every 24 hours until lesions are controlled, then tapered slowly to reach the lowest every other dose that controls clinical signs
- Isotretinoin or Acetretin
- 1 mg/kg by mouth every 12-24 hours until lesions are improved, then tapered to every 24-48 hours or 0.5mg/kg every 24 hours
- Liver enzyme values should be monitored every 2 weeks during induction
- Requires extensive owner consent to be prescribed
- Cyclosporine (Atopica)
- 5 mg/kg by mouth every 24 hours
- This is the only treatment which has may lead to an increase in sebaceous glands in addition to clinical improvement
- Vitamin A
- Treatment with appropriate antibiotics or antifungals if secondary bacterial or yeast infection is present
- Early diagnosis and treatment often leads to a better long term prognosis
Comments
- Sebaceous adenitis is inherited as an autosomal recessive condition in Standard Poodles and Akitas, therefore affected dogs should not be bred
- Sebaceous adenitis is a condition where sebaceous glands become inflamed and are eventually destroyed
- Definitive diagnosis is made via skin biopsy and dermatohistopathology
- Shorter-coated dogs may have milder clinical signs, leading to a better prognosis than longer-coated dogs.
- Some dogs have periods of spontaneous improvement and worsening that occurs independently of treatment
- Multiple therapies may be necessary to treat this condition
- Hnilica KA. Sebaceous Adenitis. In: Small Animal Dermatology- A Color Atlas and Therapeutic Guide. 3rd Edition. St. Louis: WB Saunders, 2011. p 382-384.
- Miller WH Jr, Griffin CE, Campbell KL. Granulomatous Sebaceous Adenitis. In: Muller and Kirk's Small Animal Dermatology. 7th edition. Philadelphia: WB Saunders; 2013. p. 695-699.
- www.offa.org/sa_info.html (information regarding the Orthopedic Foundation for Animals registry for Sebaceous Adenitis)
abscess
A discrete swelling containing purulent material, typically in the subcutis
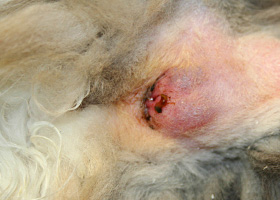
Perianal abscess in a dog
alopecia
Absence of hair from areas where it is normally present; may be due to folliculitis, abnormal follicle cycling, or self-trauma
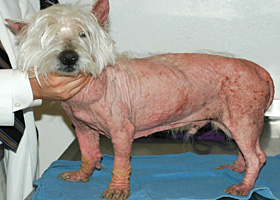
Extensive alopecia secondary to cutaneous epitheliotropic lymphoma
alopecia (“moth-eaten”)
well-circumscribed, circular, patchy to coalescing alopecia, often associated with folliculitis
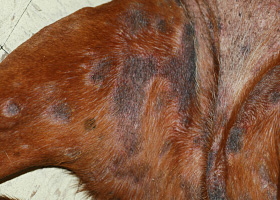
“Moth-eaten” alopecia secondary to superficial bacterial folliculitis
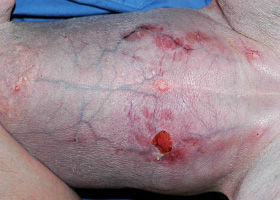
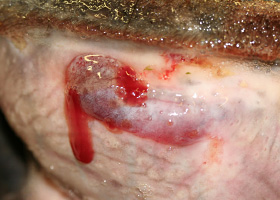
hemorrhagic bullae
Blood-filled elevation of epidermis, >1cm
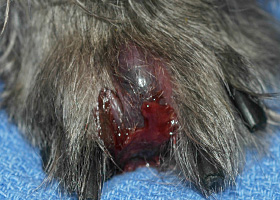
Interdigital hemorrhagic bulla in a dog with deep pyoderma and furunculosis
comedo
dilated hair follicle filled with keratin, sebum
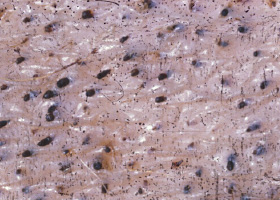
Comedones on the ventral abdomen of a dog with hypercortisolism
crust
Dried exudate and keratinous debris on skin surface
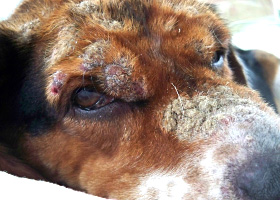
Multifocal crusts due to pemphigus foliaceus
epidermal collarettes
Circular scale or crust with erythema, associated with folliculitis or ruptured pustules or vesicles
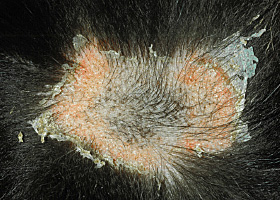
Epidermal collarettes in a dog with Staphylococcus superficial bacterial folliculitis
erosion
Defect in epidermis that does not penetrate basement membrane. Histopathology may be needed to differentiate from ulcer.
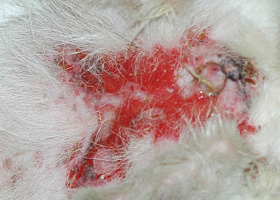
Erosions in a dog with vasculitis
erythema
Red appearance of skin due to inflammation, capillary congestion
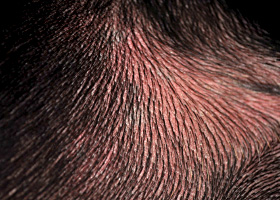
Erythema in a dog with cutaneous drug eruption
eschar
Thick crust often related to necrosis, trauma, or thermal/chemical burn
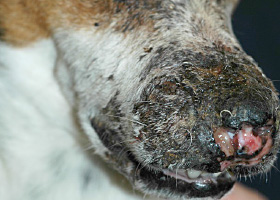
Eschar from physical trauma
excoriation
Erosions and/or ulcerations due to self-trauma
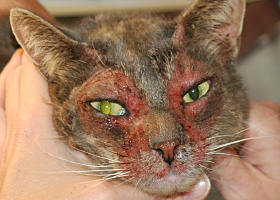
Excoriations in a cat with atopic dermatitis
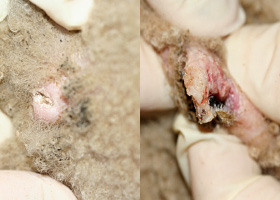
fissure
Excessive stratum corneum, confirmed via histopathology. This term is often used to describe the nasal planum and footpads.
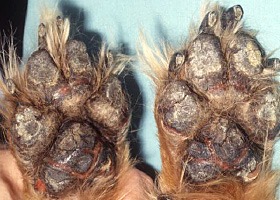
Fissures of the footpads in a dog with superficial necrolytic dermatitis
fistula
Ulcer on skin surface that originates from and is contiguous with tracts extending into deeper, typically subcutaneous tissues
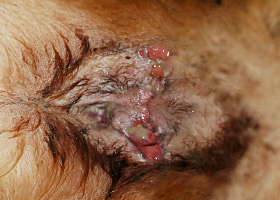
Perianal fistulas in a dog
follicular casts
Accumulation of scale adherent to hair shaft
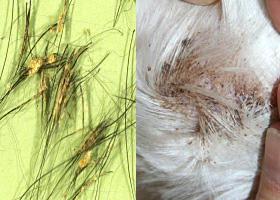
Follicular casts surrounding hairs from a dog with hypothyroidism
hyperkeratosis
Excessive stratum corneum, confirmed via histopathology. This term is often used to describe the nasal planum and footpads.
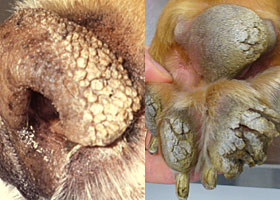
Idiopathic hyperkeratosis of the nasal planum (left) and footpads (right)
hyperpigmentation
Increased melanin in skin, often secondary to inflammation
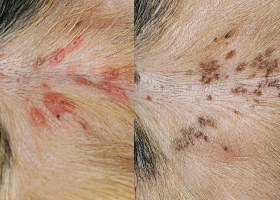
Inflammatory lesions (left) resulting in post-inflammatory hyperpigmentation (right)
hypotrichosis
Lack of hair due to genetic factors or defects in embryogenesis.

Congenital hypotrichosis in chocolate Labrador puppies.
lichenification
Thickening of the epidermis, often due to chronic inflammation resulting in exaggerated texture
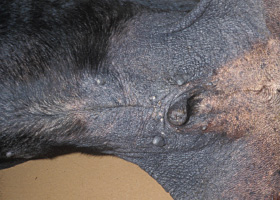
Lichenification of skin in a dog with chronic atopic dermatitis and Malassezia dermatitis
macule
Flat lesion associated with color change <1cm
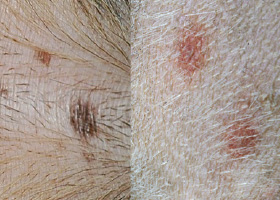
Pigmented macule (left) Erythematous macule (right)
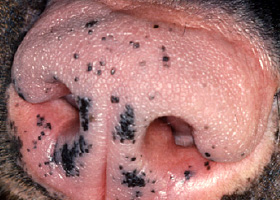
melanosis
Increased melanin in skin, may be secondary to inflammation.
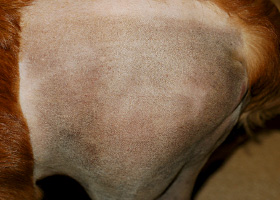
Post inflammatory hyperpigmentation of this dog’s thigh
miliary
Multifocal, papular, crusting dermatitis; a descriptive term, not a diagnosis
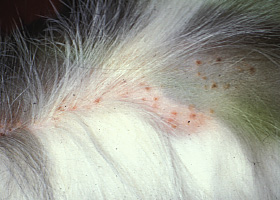
Miliary dermatitis in a flea allergic cat
morbiliform
A erythematous, macular, papular rash; the erythematous macules are typically 2-10 mm in diameter with coalescence to form larger lesions in some areas
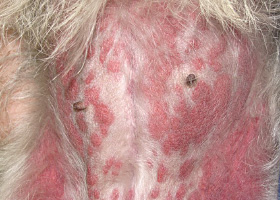
Morbiliform eruptions in a dog with a cutaneous drug reaction
onychodystrophy
Abnormal nail morphology due to nail bed infection, inflammation, or trauma; may include: Onychogryphosis, Onychomadesis, Onychorrhexis, Onychoschizia
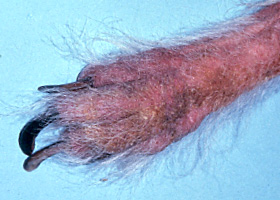
Onychodystrophy in dog with chronic allergies
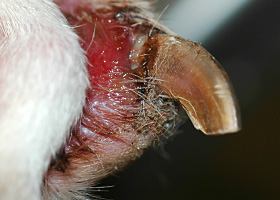
onychogryphosis
Abnormal claw curvature; secondary to nail bed inflammation or trauma

Onychogryphosis in a dog with symmetric lupoid onychodystrophy
onychomadesis
Claw sloughing due to nail bed inflammation or trauma
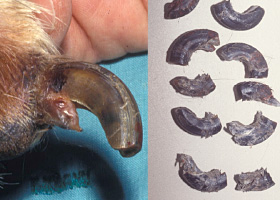
Onychomadesis in a dog with symmetric lupoid onychodystrophy
onychorrhexis
Claw fragmentation due to nail bed inflammation or trauma
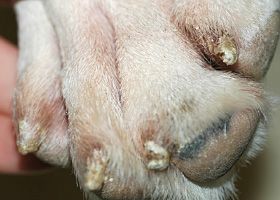
Onychorrhexis in a dog with symmetric lupoid onychodystrophy
onychoschizia
Claw splitting due to nail bed inflammation or trauma
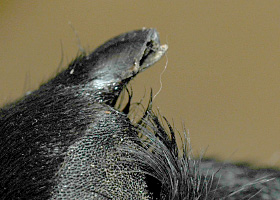
Onychoschizia in a dog with symmetric lupoid onychodystrophy
patch
Flat lesion associated with color change >1cm
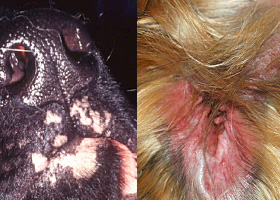
Hypopigmented patch (left), erythematous patch (right)
petechiae
Small erythematous or violaceous lesions due to dermal bleeding
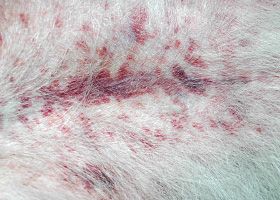
Petechiae in a dog with cutaneous vasculitis
phlebectasia
Venous dilation; most commonly associated with hypercortisolism
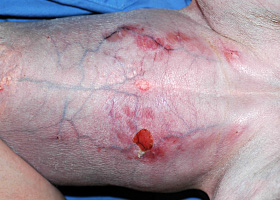
Phlebectasia and cutaneous atrophy due to hypercortisolism in a dog
plaques
Flat-topped elevation >1cm formed of coalescing papules or dermal infiltration
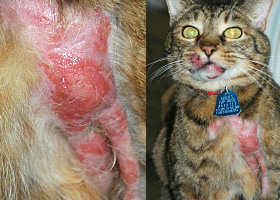
Plaques in a cat with cutaneous lymphoma
pustule
Raised epidermal infiltration of pus
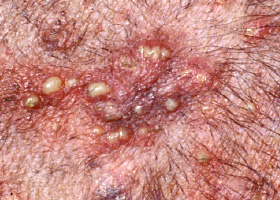
Pustules on the abdomen of a dog with superficial staphylococcal pyoderma.
scale
Accumulation of loose fragments of stratum corneum
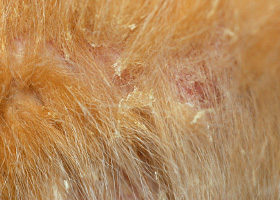
Loose, large scales due to ichthyosis in a Golden Retriever
scar
Fibrous tissue replacing damaged cutaneous and/or subcutaneous tissues
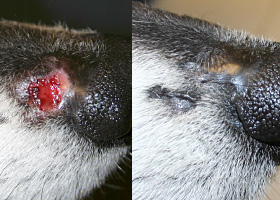
Scarring (right) following the healing of an ulcer (left) in a dog with sterile nodular dermatitis
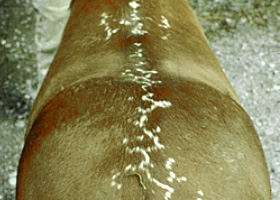
serpiginous
Undulating, serpentine (snake-like) arrangement of lesions

Serpiginous urticarial lesions on a horse
telangiectasia
Permanent enlargement of vessels resulting in a red or violet lesion (rare)
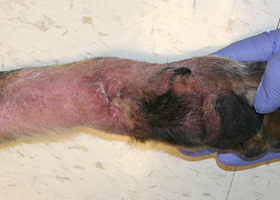
Telangiectasia in a dog with angiomatosis
ulcer
A defect in epidermis that penetrates the basement membrane. Histopathology may be needed to differentiate from an erosion.
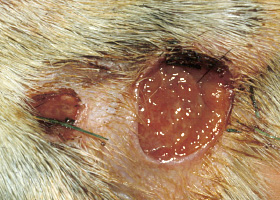
Ulcerations of the skin of a dog with vasculitis.
urticaria
Wheals (steep-walled, circumscribed elevation in the skin due to edema ) due to hypersensitivity reaction

Urticaria in a horse
vesicle
Fluid-filled elevation of epidermis, <1cm
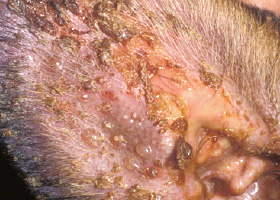
Vesicles and bullae on ear pinna due to bullous pemphigoid
wheal
Steep-walled, circumscribed elevation in the skin due to edema

Wheals associated with intradermal allergy testing in a horse